Getting AHEAD of Health Care’s Cost Growth
The Biden Administration’s new model could be CMMI’s most ambitious undertaking yet
On September 5, 2023, the Centers for Medicare & Medicaid Services (CMS) announced a new model under the Center for Medicare & Medicaid Innovation (CMMI) called The States Advancing All-Payer Health Equity Approaches and Development Model (AHEAD). This model will build on three ongoing CMMI experiments: the Vermont All Payer ACO Model, the Pennsylvania Rural Health Model, and the Maryland Total Cost of Care Model to offer versions of these models to other states. AHEAD allows for pathways similar to each of these models in important ways, but they all share one exciting element in common — the chance to rein in the costs of commercial insurance. In what follows, I will explain these models, how they each attempt to rein in health care spending, and why this could be CMMI’s most ambitious experiment ever.
Background
Medicare, Medicaid, and other payers used to all be paid on a fee-for-service (FFS) system. This style of reimbursement pays providers per service, so providers will get paid more the more services they offer and the more patients they see. This creates a perverse incentive for providers to offer pricier treatments than necessary and more of them. Because of this, some people began to advocate for value-based care where reimbursement could be tied to quality outcomes; bundled payment where providers were paid on the average episode of care rather than each service; or capitation with a lump sum payment on a fixed timeline to offer all necessary services for a population.
Medicaid Managed Care and Medicare Advantage use a version of capitation and greater control over patient care to achieve some version of reimbursement without pure FFS. Traditional Medicare has progressively switched from FFS towards bundled payment and accountable care organizations (ACOs) that emulate capitation to various degrees, whether through voluntary participation and bonus payments or bonus payments and the risk of penalties for missing quality or price benchmarks.
Aside from these options, some countries control costs by making sure hospitals charge the same rate regardless of insurance type, called all payer rate setting. This could be done either by the government setting rates directly or by negotiations between provider and insurer representatives. Other than via all payer rate setting, governments can also aim for cost savings by giving hospitals fixed annual budgets to care for all patients, called global budgets.
Vermont’s All Payer Model
This model was developed in 2017, building off the creation of the Green Mountain Care Board in 2011. This board is an independent entity responsible for overseeing the development and implementation of health care payment and delivery system reforms designed to control the rate of growth in health care costs and maintain health care quality in the state. The Board’s regulatory authority includes payment and delivery system reform oversight, provider rate-setting, health information technology plan approval, workforce plan approval, hospital and ACO budget approval, insurer rate approval, certificate of need issuance, and oversight of the state’s all-payer claims database.
After years of work, the Vermont All Payer Model was developed statewide with the intention of getting 70% of all insured residents and 90% of Medicare beneficiaries involved in an ACO by 2022. This model was introduced statewide with voluntary participation among eligible providers accepting Medicare, Medicare Advantage, Medicaid, and commercially insured enrollees. Though they have only reached 54% of Medicare enrollees in the state and a little less than 4 of 10 residents state-wide, Medicaid plans have a higher ACO participation rate at 79%. However, of the 15 eligible hospitals, 8 participated in the Medicare initiative, 14 in the Medicaid ACOs, 14 in Commercial ACOs, and 8 in all three initiatives. Additionally, 78% of practitioners were involved in any ACO in this model and 44% in all three. Only OneCare Vermont is a true all-payer ACO, and the rest are engaged in ACO initiatives in different payment schemes including the commercial sector. These ACOs use annual prospective budgets for their covered populations using past historical spending.
The Vermont All Payer Model hopes to limit annualized per capita spending growth to 3.5% each year across all payers, and limit Medicare per capita spending growth to 0.1-0.2 percentage points below the national average. Furthermore, it focuses on quality of care measures among four priorities: substance use disorder, suicides, chronic conditions, and access to care. These categories are accessed on Population-level Health Outcomes Measures and Targets, Health Care Delivery System Measures and Targets, and Process Milestones.
As a result of this model, net Medicare spending per member per year has dropped by $1,143 (9.7%), acute care stays are down 18.7%, primary care evaluation & management is up 17%, and specialty care evaluation and management visits are down 25.8%.
Pennsylvania’s Rural Health Model (PARHM)
This model began in 2019, and set prospective annual budgets for hospital inpatient and outpatient departments, global budgets regardless of volume, for Medicare, Medicaid, and some commercial patients based on hospital historical spending for 18 participating rural hospitals in Pennsylvania. These hospitals are almost evenly split between independent hospitals and hospitals in larger systems. Rather than relying on volume to meeting their needs, this model would allow for stability in revenue while removing perverse incentives to overutilize care in FFS payment schemes. PARHM had a goal of meeting 90% of hospital revenue makeup by 2020, and an annual hospital budget growth target of 3.38% per year to match Pennsylvania’s average state GDP growth rate from 1997 to 2015 with an eventual goal of $35 million in cumulative savings. Additionally, PARHM is evaluated on increasing access to primary and specialty care; reducing rural health disparities through improved chronic disease management and preventive screenings; and decreasing deaths from substance use disorder and improving access to treatment for opioid abuse.
Though the original hope was for 30 hospital participants at a minimum and greater coordination between payer types than has occurred, this model is ongoing and trying to meeting its initial goals. The pandemic may have set progress in the program back, as has hospital system hesitation to participate when not all hospitals in their system are eligible to participate.
Maryland’s Total Cost of Care Model (TCOC)
The Maryland TCOC program began in 2019, and builds on the Maryland All Payer Model that began in 2014. The Maryland All Payer Model set uniform rates for hospital reimbursement regardless of payer. The Maryland TCOC Model expanded this payment system to the outpatient setting and is conducted in three parts. Its Hospital Payment Program set population-wide hospital specific global budgets each year based on historical hospital setting. The Care Redesign Program allows hospitals to use global budget savings to make incentive payments to nonhospital health care providers who partner with the hospital and perform care redesign activities aimed at improving quality of care. This program must be entered into with CMS and the State of Maryland. Finally, the Maryland Primary Care Program is structured to incentivize primary care practices and federally qualified health centers (FQHCs) in Maryland to offer advanced primary care services to their patients. Participating practices and FQHCs will receive an additional per beneficiary per month payment directly from CMS intended to cover care management services. CMS also offers a performance-based incentive payment to health care providers intended to incentivize them to reduce the hospitalization rate and improve the quality of care for their attributed Medicare beneficiaries, among other quality and utilization-focused improvements. Starting in 2023, this program introduced upside and downside risk to enforce greater accountability on provider targets.
Nearly every hospital in Maryland, 52 total, participated in the TCOC model, and 85% participated in some episode incentive program. Of Maryland’s primary care clinics, 27% voluntarily participated in the model. Maryland’s TCOC model is the most comprehensive of the three models because it combines global hospital budgets in the inpatient and outpatient setting with all payer rate setting in a market that almost entirely complies with the program, and an optional primary care model within it that more than a quarter of primary care clinics participate in as well.
As a result of the TCOC model, Maryland decreased per enrollee Medicare spending by as much as $450 in 2019 to $162 in 2021 during the pandemic. From 2019-2021, total hospital spending decreased by around 5%, hospital admissions by 15%, outpatient emergency department visits by 5%, preventable admissions by 15%, and 30-day unplanned readmissions by 10%; all in larger magnitude than the previous All Payer Model. Though there was an increase in non-hospital spending, savings in hospital spending more than offset it for a total savings of $781 million from 2019 through 2021, almost halfway to the model’s target of $2 billion in savings in its eight-year program. This was achieved without harming patients during the pandemic.
States Advancing All-Payer Health Equity Approaches and Development Model (AHEAD)
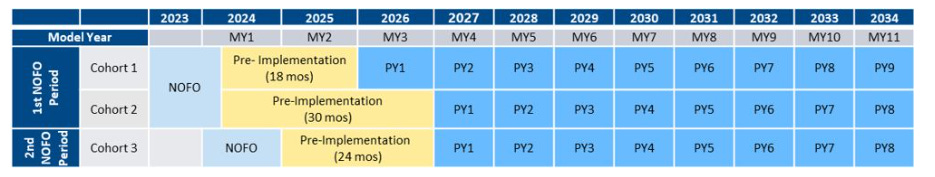
The AHEAD model will last from 2024 through 2034, 11 years total, with the first cohort of hospitals beginning their first proper performance period in 2026. AHEAD is another TCOC model that aims to curb health care cost growth, improve overall state population health among participants, and reduce disparities in health care outcomes among underserved populations. Up to eight states will be able to participate in this program and will be approved by CMS based on their perceived ability to implement the AHEAD model well.
This model will use inpatient and outpatient hospital budgets just as all three of the models described previously. States will be able to apply for this program to be entirely state-wide, like Maryland or Vermont, or to a specific region, like PARHM. Budgets for hospitals will be prospective and quality of care targets will be used for all participant hospitals. All payer cost growth targets include Traditional Medicare, Medicare Advantage, Medicaid, and commercial plans. Commercial participants must include at least state employee health plans, qualified health plans on the individual marketplace, or other commercial payers. Quality of care and population health targets to be measured will be selected by states from a menu of options. Primary Care AHEAD emulates Maryland’s TCOC voluntary add-on for primary care clinics, and participating clinics in this model will be required to align care for their Medicaid enrollees.
The AHEAD model could be on a spectrum in states from regional voluntary hospital participation like in Pennsylvania, to statewide voluntary ACO programs that are not true all payer like Vermont, or nearly universally participating hospitals in all payer schemes with global budgets and substantial primary care participation like Maryland. These three states can either apply for AHEAD or continue with their current approved models and hope for an extension.
Why does this matter?
Over the course of CMMI’s first 12 years, most models have been specific to Traditional Medicare enrollees, with only a handful like Financial Alignment Initiative (FAI) or others aimed at Medicare-Medicaid enrollees, Medicaid enrollees, or Medicare Advantage enrollees. Even fewer put any sort of pressure on more than one type of plan or commercial plans, and often they are voluntary when they do so. Even among mandatory programs outside of CMMI written in the Affordable Care Act (ACA), they tend to be directed only at one or two quality measures among the Medicare population. Combining hospital global budgets, primary care incentives, payer alignment (including commercial payers!), and health equity and quality benchmarks in up to 8 states could drastically expand the number of states that try to hold down costs outside of what is traditionally thought of as “public” insurance. This will be done trying to reduce health disparities and improve population health as well, a goal of equal importance to cost containment itself. Bringing all three goals together, consolidating payment amounts between payers and moving away from FFS towards a capitated model could avoid disincentives to accepting Medicaid patients and increase predictability in provider budgets. Coming off a pandemic that killed over one million Americans in some part due to a fractured health care system, a direct focus on reducing health care disparities, improving population health, and removing disincentives for taking the patients of the most need is incredibly important.
If this model works, it could finally bend the commercial market cost curve just like the United States has been attempting to do so in Medicare and Medicaid since the passage of the ACA. And with a successful model, Health and Human Services (HHS) could expand the model nationally or to a lesser extent as they have done with models in the past. Anyone interested in health policy should be watching this model closely.